Premenstrual syndrome, also called PMS, changes mood and emotions, physical health, and behavior between ovulation and the start of your period, roughly estimated to be two weeks before your period. It lasts until a few days after your period begins and shows up consistently each month.
PMS is a widespread concern. About 48 percent of women of reproductive age experience PMS, and symptoms are severe in about 20 percent, enough to affect their daily routine.
PMS is an actual condition that can derange everyday life and cause considerable physical discomfort and emotional distress.
Causes of Premenstrual Syndrome
There is no definitive cause and explanation for why some people experience PMS more severely than others. As per Robert F Casper, MD Professor, Division of Reproductive Sciences, PMS is a group of physical and behavioral symptoms, whereas MD Rick D. Kellerman emphasizes correct diagnosis of the PMS symptoms before treatment.
Let’s know the other current theories around PMS:
Cyclical changes in hormones
Dr. Rick thinks PMS occurs in reaction to changing hormones estrogen and progesterone levels. These hormones naturally vary throughout your menstrual cycle. During the luteal phase, hormones peak and decline rapidly, which may lead to anxiety, irritability, and other mood changes.
1. Chemical changes in the brain
Chemical messengers such as neurotransmitters serotonin and norepinephrine may factor into symptoms of PMS as they have several essential functions in the body, including helping regulate mood, emotions, and behavior.
For example, a decrease in estrogen may stimulate the release of norepinephrine, leading to the declining production of dopamine, acetylcholine, and serotonin. These changes can start sleep issues and lead to a low or depressed mood.
2. Lifestyle factors
Few lifestyle factors might affect the severity of your PMS symptoms. Potential factors that could exacerbate PMS symptoms include:
- smoking
- a lack of quality sleep
- eat a lot of meals high in sugar, fat, and salt
- alcohol consumption
- a lack of regular physical activity
3. Existing mental health conditions
If you have mental health conditions, such as depression or anxiety could increase your possibility of experiencing PMS or premenstrual dysphoric disorder (PMDD).
Life Changing Experiences with Aastha Fertility - From Doubt to Success
A family history of PMS, depression, postpartum depression, or bipolar disorder can also increase this risk.
You might also notice premenstrual worsening. It means symptoms of underlying mental health conditions, like bipolar disorder or depression, intensify shortly before your period begins.
There is no conclusive explanation linking mental health symptoms and menstruation-related mood changes. But many think it associates with the chemical changes in the brain.
Symptoms of PMS
Though PMS causes mild to moderate symptoms that don’t major impact daily life, they can become painful enough to interfere with your everyday activities and overall health.
You will experience symptoms unfailingly before each menstrual period if you have PMS. You might have only some of the following symptoms or several, but PMS generally involves at least a few different symptoms.
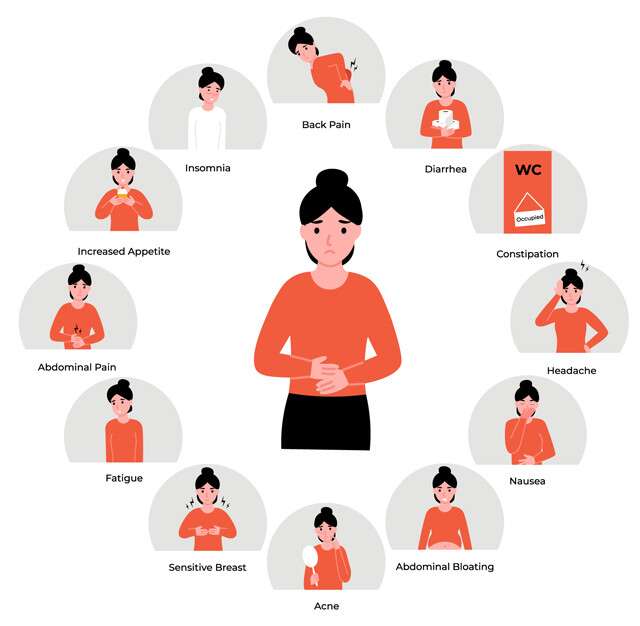
1. Physical symptoms
With PMS, you will likely also notice some physical symptoms, such as:
- abdominal bloating
- cramping
- headaches
- unusual sensitivity to light or sound
- sore and swollen breasts
- acne
- constipation
- diarrhea
- back and muscle pain
- unusual clumsiness
2. Emotional and behavioral symptoms
PMS-related shifts in your emotions, mood and behavior might include:
- unusual anger and irritability
- anxiety, restlessness, or feeling on edge
- modifications in sleep patterns, including fatigue and trouble sleeping
- reduced sex drive
- change in appetite, which includes increased food cravings, specifically for sweets
- a low or sad mood, which might involve tearfulness or sudden, uncontrollable crying
- rapid changes in mood and emotional outbursts
- difficulty concentrating or remembering information
Could It Be Premenstrual Dysphoric Disorder
Watch this video to learn more about PMDD.
The premenstrual dysphoric disorder is a severe form of PMS.
As with PMS, PMDD symptoms may occur due to fluxes in estrogen, progesterone, and serotonin levels.
3. Symptoms of PMDD might include:
- thoughts of suicide
- depression, intense sadness, and crying spells
- panic attacks
- a lack of interest in daily activities
- anxiety, anger, or irritability
- insomnia
- trouble thinking or focusing
- sudden shifts in mood
- binge eating
- painful cramping
- bloating
When To Contact a Doctor To Help With PMS?
If you have tried all things but still have lousy PMSing, it’s probably time to get help. Consult with our doctor or gynecologist. They will ask about your symptoms, health, and medicines and may take blood tests to ensure the issue is PMS.
Track your mensuration cycle and make a report. It will help you get the best help from the doctor.
Premenstrual Treatment Available
Lifestyle changes can help relieve PMS symptoms for many women. Premenstrual syndrome can also be treated with one or more medications, depending on the severity of your symptoms. Women experience varying degrees of success when taking medications to relieve their symptoms. You can treat premenstrual syndrome with the following medications:
- Antidepressants: Selective serotonin reuptake inhibitors have been successful in reducing mood symptoms. SSRIs are the first-line treatment for severe PMS or PMDD. These medications are supposed to be taken daily, but antidepressants may be limited to the two weeks before menstruation begins for some women with PMS.
- Diuretics. Taking diuretics can help your body shed excess fluid through your kidneys.
- Nonsteroidal anti-inflammatory drugs (NSAIDs): Taken before or at the start of your period, NSAIDs can ease cramping and breast discomfort.
- Hormonal contraceptives. These prescription medications may bring relief from PMS symptoms by stopping ovulation.
Lifestyle and home remedies
Sometimes symptoms of PMS could be managed or reduced by making changes in your everyday lifestyle. The following tip from our Senior Gynecologist Namita Kotia, could be helpful:
#1 Modify your diet
- Eat less, more frequent meals to reduce bloating.
- Limit salt and salty foods for decreasing bloating and fluid retention.
- Avoid caffeine and alcohol.
- Eat foods high in complex carbohydrates.
- Choose foods rich in calcium.
#2 Incorporate exercise into your routine
Participate in brisk walking, cycling, swimming, or another aerobic activity for at least 30 minutes. Regular exercise can help enhance your overall health and relieve specific symptoms, such as weariness and a depressed mood.
#3 Reduce stress
- Get plenty of sleep.
- Try progressive muscle relaxation or deep breathing exercises to reduce headaches, anxiety, or trouble sleeping.
- Try yoga or massage to de-stress.
#4 Record your symptoms for a few months
Identify the triggers and keep a record of them to strategize how to lessen them.
Conclusion
PMS is a prevalent condition. Some women have to face very severe effects while others do not. Consult our doctor if you are going through severe PMS and have tried all the remedies. There are a few medications that could help you with the symptoms.







Leave a comment