
At Aaastha fertility we believe in transparency with counseling with respect to

Defined as failure to achieve pregnancy within 12 months of unprotected intercourse or therapeutic donor insemination in women younger than 35 years.
Women older than 35 years after 6 months of failed attempts to become pregnant or earlier, if clinically indicated.
In women older than 40 years, more immediate evaluation and treatment.
If a woman has a condition known to cause infertility, the obstetrician–gynecologist should offer immediate evaluation.
Initial workup includes a review of the medical history, physical examination.
Female Partner: tests will focus on ovarian reserve, ovulatory function, and structural
Abnormalities: Hormone profile [AMH, FSH, LH, ESTRADIOL, etc], Transvaginal Sonography [TVS], Tubal Patency Tests [HSG, SSG]
Male factor: medical history and physical examination, Semen Analysis, Scrotal Sonography [TRUS].
Done under short General Anaesthesia.
For oocyte retrieval during IVF, Simple ovarian cyst aspiration.
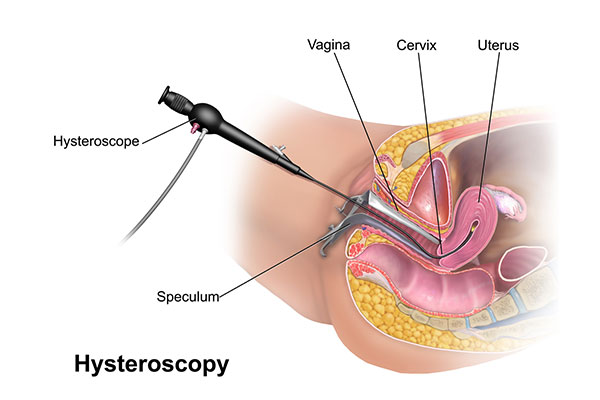
Hysteroscopy is considered the gold standard for evaluating the uterine cavity, and due to improved endoscopic developments.
Hysteroscopy is used as a therapeutic method in many conditions that may affect fertility, such as symptomatic uterine septum, intrauterine adhesions, endometrial polyps, sub mucous leiomyomas.
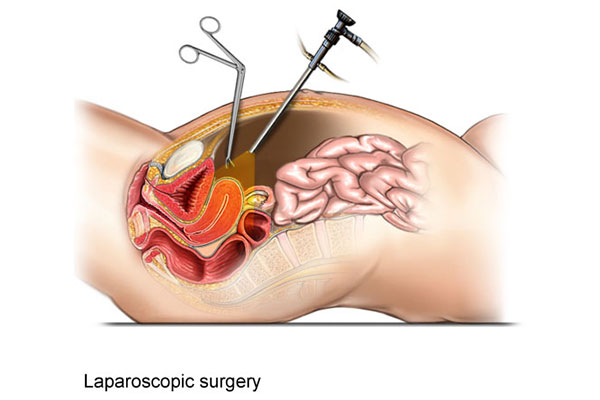
Laparoscopy for infertility is a minimally invasive surgical procedure that uses a laparoscope (a fiber-optic tube with light and video camera) inserted through two or more minor incisions, often in the belly button. The surgeon can then visually examine the pelvic reproductive organs and the pelvic cavity.
Diagnostic laparoscopy is useful in demonstrating tubal patency, tubo- ovarian relation, pelvic adhesions, peritoneal diseases, endometriosis and fibroids.
Operative Laparoscopy for fibroids, endometriosis, adhesiolysis, benign ovarian cysts and fallopian tube recanalisation.
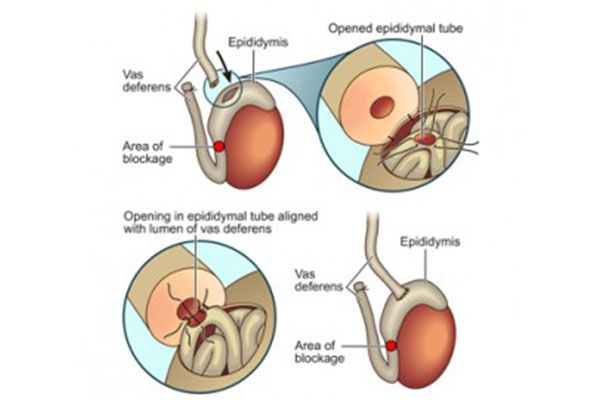
Indicated for idiopathic epididymal obstruction, secondary epididymal obstruction due to long-standing vasal obstruction, or iatrogenic epididymal obstruction following interventions such as epididymal aspiration or reversal of vasectomy [male sterilization].
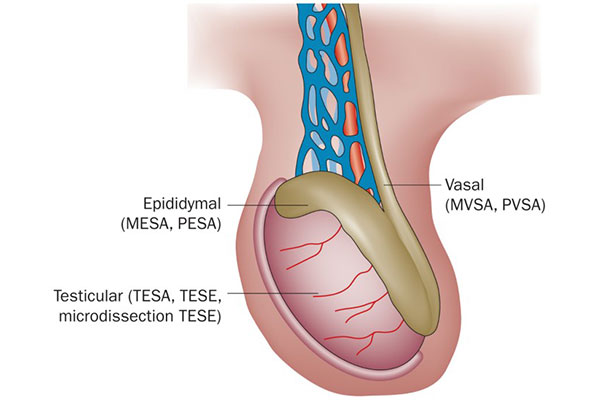
Used in the setting of post-vasectomy obstruction, CBAVD, ejaculatory duct obstruction (EDO), and unreconstructable causes of obstructive azoospermia.
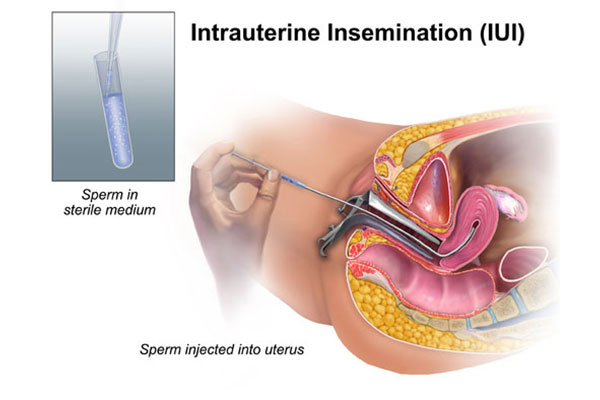
Intrauterine insemination is a procedure that places sperms past the cervix and in a woman’s uterus around the time of ovulation.
This procedure makes the passage to fallopian tubes much shorter and there is a better chance that more sperms will encounter the egg.
Female Factors:
Male Factor:
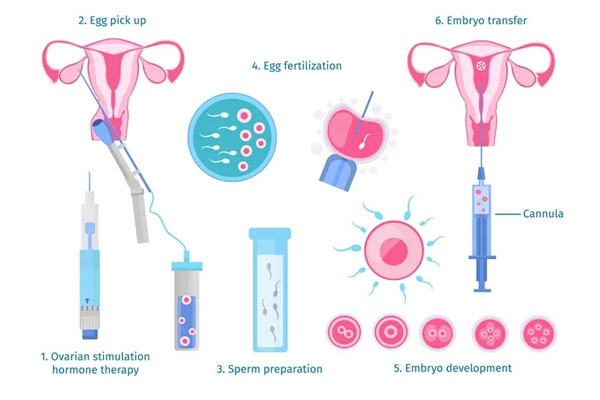
Indicated in:
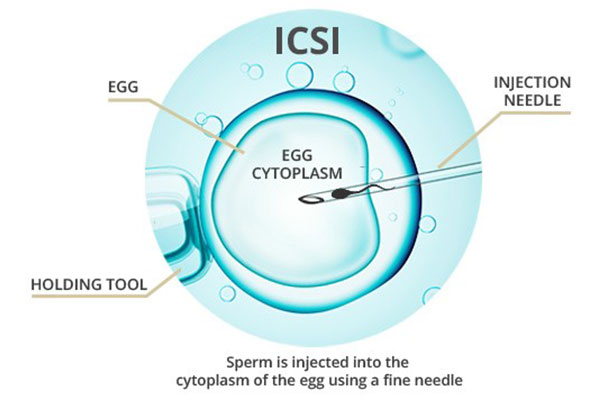
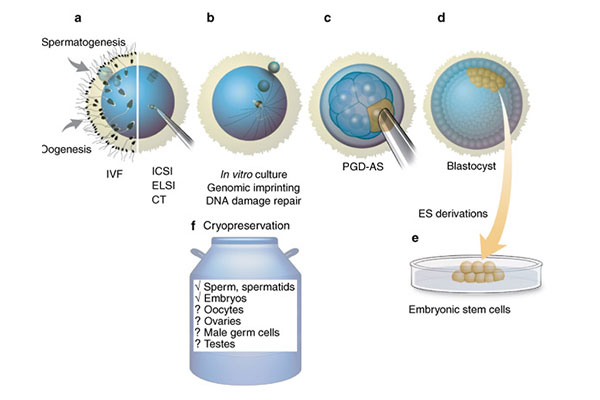
Intracytoplasmic sperm injection (ICSI) is the procedure during which an embryologist injects a single sperm directly into the woman’s egg as part of the in vitro fertilization (IVF) procedure to aid in fertilization.

A high-risk pregnancy is one that threatens the health or life of the mother or her fetus. It often requires specialized care from specially trained providers.
Risk factors for a high-risk pregnancy can include:
By definition, “recurrent” pregnancy loss is defined as the loss of two or more pregnancies from the time of conception until 24 weeks of gestation. At Aastha fertility care we provide TREATMENT PLAN, SUPPORTIVE CARE AND PSYCHOLOGICAL CARE.
Refers to cases in which women have had three failed in vitro fertilization (IVF) attempts with good quality embryos.
Fill out the form below, and we will be in touch shortly.